Highlights:
- Since the second wave started on March 1, Mumbai has recorded 2,784 deaths.
- Mumbai has equipped its hospitals with pipes that supplied oxygen directly to patients’ beds.
- Since more children could be contaminated in the next surge, Mumbai’s municipality is planning for a third wave by establishing paediatric hospitals.
- Even the Supreme Court has stated that elements of the Mumbai model can be implemented in other cities.
As the deadly new coronavirus swept India, Mumbai Municipal Commissioner Iqbal Singh Chahal was informed at 12 a.m. on April 17 that six hospitals in his city would run out of oxygen within hours, putting 168 patients’ lives in jeopardy.
Also Read: Army Of The Dead” Premiers In US Theaters, “Radhe” Shunned By Indian Cinemas
The patients were rushed to the temporary hospitals set up by Iqbal Singh Chahal’s team during the city’s first wave in 2020 amid the ensuing chaos. Even when the cases dropped, he hadn’t dismantled the facilities. They were fitted with pipes that delivered oxygen directly to patients’ beds, unlike most hospitals that relied on cylinders. All 168 people made it out alive.
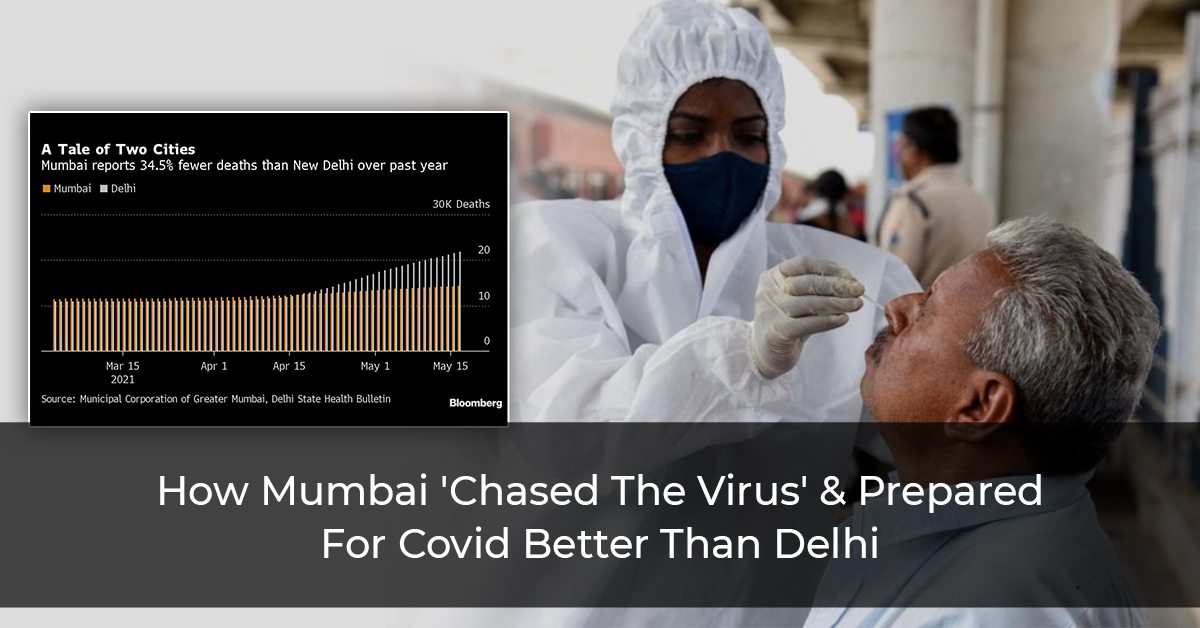
That night, which Iqbal Singh Chahal describes as the scariest he’s ever seen, gave insight into the strategies Mumbai employed to control the outbreak faster and with less casualties than other parts of the country. Since the second wave started on March 1, Mumbai has recorded 2,784 deaths, accounting for about a quarter of the 10,595 deaths in New Delhi. The Supreme Court has also proposed that aspects of Mumbai’s model could be implemented in other parts of the country, such as New Delhi.
By contrast, India continued to report a record number of daily deaths, as well as the breakdown of the health system in some parts of the country, have exposed widespread governance and public planning flaws across the country.
The city’s success, according to Iqbal Singh Chahal, can be attributed to a decentralised structure set up by his team during the first wave, which included neighbourhood war rooms to handle cases by place. He’s also changed the way the city gets and uses medical oxygen, creating emergency stocks and tracking systems for tankers. As a result, even as families cried out for supplies on social media, Mumbai’s patients registered fewer issues.
Mumbai is the world’s second-most densely packed city, according to UN statistics, with a population of 16 million people spread across gleaming skyscrapers, apartment complexes, and sprawling slums. There are approximately 32,000 people per square kilometre.
“I knew it was going to be a long fight, and I knew only systems could win wars — individuals couldn’t,” Chahal said in a Zoom interview. “The Mumbai model is heavily reliant on system design and automation.”
Mumbai had nearly half the number of active virus cases as New Delhi as of May 11. Satyendar Jain, the Delhi Health Minister, and Ashish Chandra Verma, the Principal Secretary of Health, did not return calls seeking comment.
The threats to Mumbai, however, are far from over. Since the outbreak started, the city has reported 688,696 cases, with 1,544 more on May 16. Iqbal Singh Chahal is planning for a third wave by establishing jumbo paediatric hospitals, citing public health experts’ warnings that the next surge could result in more children being contaminated.
Given the possible human toll of a runaway outbreak, controlling the virus’s trajectory in Mumbai is critical. In addition, as India’s financial hub, the city is critical to the country’s still ailing economy.
The country’s main stock exchange is located in Mumbai. It’s home to big multinationals like Unilever Plc and global financial behemoths like Citigroup Inc. and KKR & Co. It is home to the country’s central bank as well as Bollywood, the world’s largest film industry.
Iqbal Singh Chahal, 55, credits his managerial abilities to his upbringing in a military family: His father served in the Indian army as an officer. He’s held a number of government jobs over the years, including working on a plan to remodel Dharavi and overseeing an expansion of Maharashtra’s irrigation systems.
When Maharashtra’s Chief Minister Uddhav Thackeray asked him to lead the municipal corporation at the height of Mumbai’s first wave, he had to hit the ground running. Bodies were piling up in morgues, and Dharavi, the city’s densest slum, was fighting a rapidly spreading coronavirus outbreak.
Last year’s lessons showed him the value of a local approach and easily isolating patients, a model he calls “Chase the Virus.” His team went door to door in Dharavi searching for people who had symptoms, finally isolating 150,000 people from the slum and breaking the infection chain. Iqbal Singh Chahal also abolished the central hub that handled the city’s crims at the time.
Last year’s lessons showed him the value of a local approach and easily isolating patients, a model he calls “Chase the Virus.” His team went door to door in Dharavi searching for people who had symptoms, finally isolating 150,000 people from the slum and breaking the infection chain. Iqbal Singh Chahal also abolished the city’s central crisis management centre and established local war rooms in each of the city’s 24 administrative divisions — wards or neighbourhoods — at the time.
Since wealthy areas were hit the hardest during the second wave, the localised approach paid off. The local war rooms received test results and directed patients to the nearest available hospital beds, reducing the spread of infection. The city council worked with private hospitals to secure beds for Covid patients at government-determined rates.
Iqbal Singh Chahal said, “We established an excellent public-private partnership between hospitals that is still not noticeable in the rest of the world.”
As oxygen became scarce during the second wave, Iqbal Singh Chahal began obtaining oxygen from neighbouring states. Mumbai’s civic authorities have made it illegal for hospitals to add beds that exceed their oxygen storage capacity, avoiding the shortages that have afflicted other cities.
Vaccinations
Dr. Hetal Marfatia, professor and head of the ear, nose, and throat department at Mumbai’s KEM Hospital, said, “Wiser after our experience last year, when the second wave struck with its hazardous mutations, the Brihanmumbai Municipal Corporation rapidly scaled up its facilities, including beds, equipments, and doctors.” She said that this time around, most hospital beds had readily accessible oxygen lines.
Iqbal Singh Chahal said he’s had to “find creative ways to use scarce resources” at times. When ambulances were scarce, he contacted the city’s election board, which converted the 800 cars sent over into ambulances by erecting partitions between the driver and the passenger.
Despite the fact that Mumbai has twice been the epicentre of the virus, local doctors warn that the threat remains. Iqbal Singh Chahal’s team has also been chastised for what some have characterised as a disorganised vaccination policy.
Dr. Vikas Oswal, a pulmonologist who practises in Dharavi and other parts of Mumbai, said, “While our cases graph has come down now, I would say this is not the end.” “Due to overcrowding at vaccination centres, we foresee a spike in cases over the next two weeks. They are not being adequately handled.”
Iqbal Singh Chahal admits some of the risks, stating that he is planning more jumbo hospitals with 6,500 additional beds and is attempting to import vaccines directly from foreign companies. “We have a greater chance of reducing the threat of the next wave if we give out more vaccines,” Chahal said